Closed Formulary Working to Drop Prescription Drug Costs
The Texas Division of Workers’ Compensation has published a report authored by the agency’s Research and Evaluation Group that analyses injured employee outcomes after the implementation of the Texas pharmacy closed formulary. The October 2019 report details the dramatic impact the closed formulary has had on patient outcomes and pharmacy costs in the Texas workers’ compensation system.
In 2011, the Division of Workers’ Compensation implemented a pharmacy closed formulary to manage drug prescriptions to injured employees. Prescriptions excluded from the formulary like investigational and experimental drugs, “not-recommended” drugs (N-drugs), and compound drugs require pre‐approval by the insurance carrier before they can be dispensed. This study looks at injured employee outcomes such as return-to-work rates and health outcomes since the formulary was implemented.
The key findings from five important areas include:
Health Outcomes Mental and physical functioning scores for network injured employees increased after the formulary. For non-network injured employees, physical functioning scores also increased, but mental functioning scores remained unchanged.
Return to Work The average return-to-work rate for network and non-network employees increased after the pharmacy closed formulary.
Medical Disputes The number of workers’ compensation medical disputes decreased significantly.
Receiving Prescriptions About 78 percent of injured employees said they had no problem receiving their prescriptions.
Medical Interlocutory Orders After accounting for withdrawn requests, 60 percent of the Medical Interlocutory Orders (MIO) requested were approved.
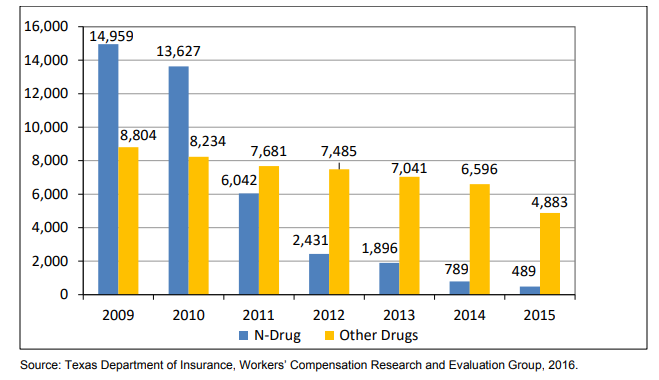
The report documents a number of changes in opioid trends from 2009 to 2015. For example, the total number of claims receiving high levels of N-drug opioids decreased from 14,959 in 2009 to 489 in 2015. Moreover, the total number of claims receiving high levels of other opioids decreased from 8,804 in 2009 to 4,883 in 2015.
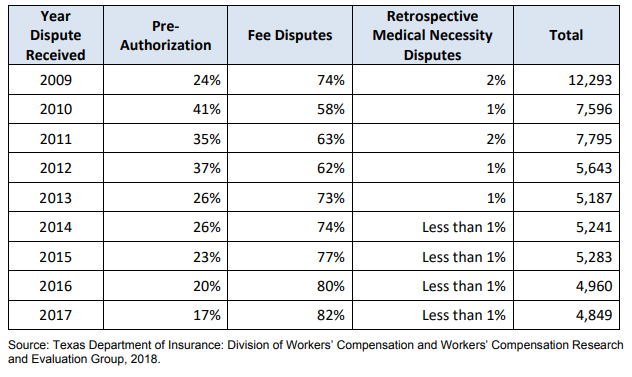
Meanwhile, the number of medical disputes filed between 2009 and 2017 have dramatically decreased. The number of workers’ compensation medical disputes decreased 38 percent from 2011 (when the formulary was implemented) to 2017. Preauthorization disputes, including disputes over N-drugs prescriptions, declined from 41 percent of all medical disputes in 2010 to 17 percent in 2017. The REG stated that the decrease in disputes is related to several factors, such as fewer claims filed, the creation of health care networks in 2006, the adoption of DWC’s medical treatment guidelines in 2007, and DWC’s adoption of professional, inpatient and outpatient hospital, and ambulatory surgical center fee guidelines in 2008.
The report concludes that as the post-formulary utilization and costs of prescriptions decreased, outcomes improved in most measures, especially for network claims. Return-to-work rates and health outcomes increased most years. Medical disputes (which include pharmacy disputes) decreased significantly, a measure of decreasing friction between injured employees and insurance carriers over fees, medical necessity services, and preauthorization. However, the 2018 survey results demonstrate that significant opportunities exist for prescribing doctors to help improve injured employee outcomes with more adherence to best practices.



