DWC Data Shows Vaccine Claims Play Small Role in COVID-19 Exposure
The most recent information received from the DWC COVID-19 data calls indicates that COVID-19 vaccine reaction claims are playing a very small part in carrier exposure following the pandemic. A recent Division report indicates that from December 15, 2020, through May 9, 2021, insurance carriers reported a total of 448 COVID-19 vaccine reaction claims to DWC. Among these 448 claims, 60 claims were reported in December 2020, 214 in January 2021, 110 in February 2021, 38 in March 2021, 24 in April 2021, and 2 in May 2021.
As of April 14, 2021, insurance carriers paid $42,254 in indemnity and medical benefits for COVID-19 vaccine reaction claims. A total of $30,919 was paid as indemnity benefits (employer salary continuation: $22,089 and temporary income benefits: $8,830) for an average of 15 days of disability per lost-time claim (median: 13 days). Similarly, insurance carriers paid a total of $11,335 as medical benefits (professional services payments: $4,216, hospital/facility payments: $6,996, and pharmacy payments: $123).
Most of the vaccine reaction claims (81%) were processed by political subdivisions, 17% by commercial carriers, and 2% by the State of Texas. The public administration industry sector represented most of the vaccine reaction claims (79%), followed by health care and social assistance sector (15%), and accommodation and food services sector (2%). To date, the vast majority of COVID-19 vaccine reaction claims filed (90%) have not been initially denied by the insurance carriers.
The findings were announced in the latest results from the Division’s mandatory data call for information related to COVID-19 injuries reported to select insurance carriers. The data call originated in Commissioner’s Bulletin No. B-0029-20 and followed the agency’s request for public comment from system stakeholders to help shape the parameters of the data call. In Commissioner’s Bulletin No. B-0003-21, DWC extended the data call through June 2021 for all selected carriers.
The Report and Key Findings
The Division has periodically released the results of earlier data call submissions though the Research and Evaluation Group. In its most recent report, COVID-19 in the Texas Workers’ Compensation System, the REG highlighted the following key findings from the data call:
Claim frequency: Although COVID-19 caused a brief shutdown for some jobs and moved others to remote work, the total number of workers’ compensation claims reported to DWC in 2020 was about 34% higher than in 2019. The increase in COVID-19 occupational disease claims reported so far has temporarily interrupted a 20-year trend in Texas of fewer workers’ compensation claims reported each year. Since new claims are still being reported, these statistics may change over time.
COVID-19 claims: From January 1, 2020, through May 9, 2021, insurance carriers reported a total of 48,663 COVID-19 claims to DWC. Figure 1 shows the number of COVID-19 claims received by insurance carriers each month. The number of COVID-19 claims began to increase starting in March consistent with Governor Greg Abbott’s COVID-19 disaster declaration in Texas. Claims began to decline in mid-April as Texas began reopening efforts, started surging in June, and continued to increase until mid-July. Claims began to decline again in mid-July through September then started to increase again in October and continued through December. Claims started declining again in January 2021 and continued to decline each month since then.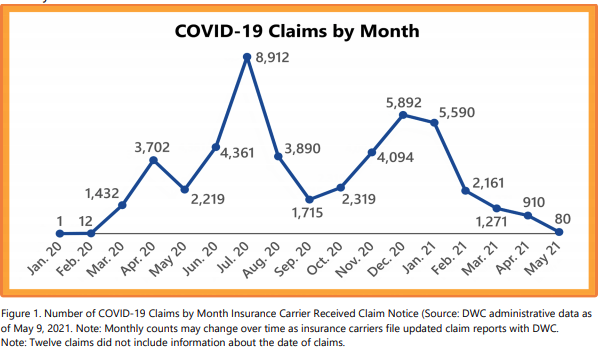
Indemnity benefits paid: Using DWC’s administrative data as of April 22, 2021, for the claims reported as of March 31, 2021, insurance carriers and employers paid $24.1 million in indemnity benefits on COVID-19 claims to date, $10.9 million (45%) in employer salary continuation, $12.9 million (53%) in workers’ compensation income benefits, $244,390 (1%) in death benefits, and $121,202 (1%) in burial benefits.
Most of these costs have been paid by political subdivisions (60%) followed by commercial insurance carriers (36%), and the State of Texas (4%). The cost of these claims payments will continue to change over time as injured employees lose time away from work, move from one income benefit type to another, or as additional death benefits are paid to legal beneficiaries.5 Injured employees receiving income benefits (i.e., employer salary continuation, temporary income benefits, and impairment income benefits) were paid for an average of 19 days of disability per lost-time claim (median: 14 days). The average income benefit payment made for the claims with injury dates from January to September 2020 was $2,145 at six months post-injury.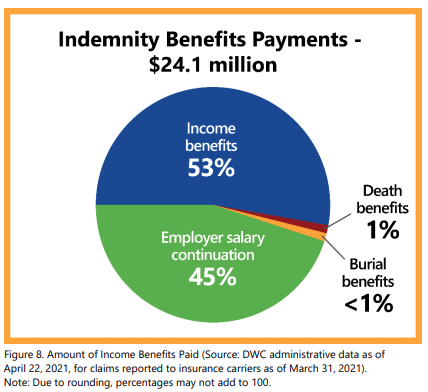
COVID-19 claims by county, occupation, gender, age, type of insurance carrier, and type of industry: The majority (61%) of the state’s COVID-19 cases were concentrated in 10 counties as of May 9, 2021. Likewise, the majority (58%) of the state’s COVID-19 workers’ compensation claims were concentrated in these same 10 counties. Nearly half (45%) of the COVID-19 claims involved first responders and correctional officers, and slightly more than half (52%) of claims were processed by the State of Texas and its political subdivisions acting as insurance carriers.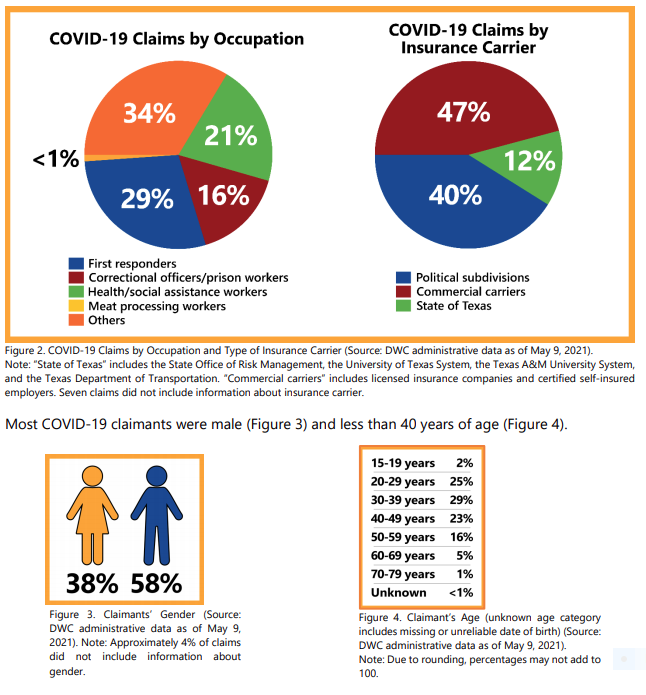
Background and Conclusions
On March 13, 2020, Texas Governor Greg Abbott issued a statewide disaster declaration for COVID-19. While state and local efforts are being made to address the pandemic, there are still many unknowns about its ultimate impact on the Texas population and economy, and on employees and employers covered under the state’s workers’ compensation system.
Early in the pandemic, DWC monitored the COVID-19 claims reported by insurance carriers and realized that many of these claims appeared to be “exposure only” claims, with no documentation of whether the injured employee tested positive for COVID-19. Many of these claims were being investigated and either accepted or denied by the insurance carrier, based on whether the injured employee could provide medical evidence of a positive test or diagnosis, as well as documentation showing a connection between the COVID-19 infection and work.
To understand the proportion of these COVID-19 claims with a positive test or diagnosis, DWC issued a data call that ultimately required data reporting from 74 insurance carriers representing the State of Texas, political subdivisions, and commercial insurance carriers.
Overall, the results of the data call (for claims reported to the insurers as of March 31, 2021), showed that 63% of the COVID-19 claims involved an injured employee who tested positive or was diagnosed with COVID-19. Among these positive test claims, nearly half (48%) were accepted as work-related by insurance carriers, half (50%) were denied by the insurance carriers, and 2% were still under investigation.
These statistics vary across types of insurance carriers. COVID-19 claims being processed by the State of Texas reported the highest rate of denials (87%); however, commercial insurance carriers had the highest number of denials. Despite the number of COVID-19 claims denied, DWC’s administrative data as of May 9, 2021, showed that there were only 85 COVID-19 claim disputes filed with DWC.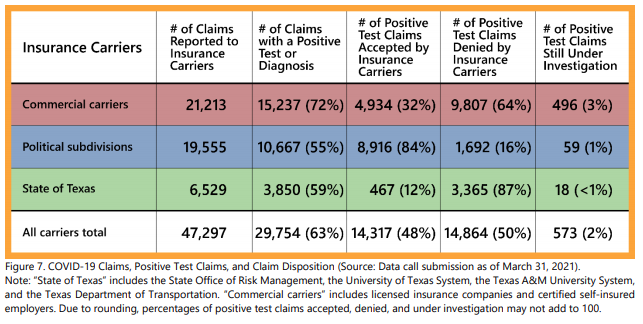
Reminder on Employer Reporting and Carrier Coding for COVID-19 Claims
Employer Reporting: In the past, Division staff has voiced concerns that they had not been seeing the reporting of as many COVID-19 claims as had been anticipated. Under Rule 120.2 (a) an employer must notify its carrier of each death or occupational disease it receives notice of, as well as any injury that results in more than one day’s absence from work. The employer must do so within eight days of receipt of this notice. Carriers must then electronically file specific information from the original Employer’s First Report of Injury not later than the seventh day after receipt of such a required report where there is lost time from work or an occupational disease. Rule 124.2(c) (1) (A).
Carrier Coding COVID-19 Claims: It is also important to remember that DWC issued the following coding guidance in a memo on March 27, 2020. DWC expects carriers to use the International Association of Industrial Accident Boards and Commissions codes for EDI claims reports: “cause of injury” code 83 -Pandemic and “nature of injury” code 83 – COVID-19 on April, 2020. We recommend that you remind those persons within your organization who are responsible for injury coding of this obligation. If the coding has been omitted on claims reported on or after April 1, 2020, we recommend going back and amending your reporting to include the proper coding.
Carrier Coding COVID-19 Vaccination Claims: In addition, on March 2, 2021, issued advice to carrier regarding their obligation to report and code claims involving adverse reactions to the COVID-19 vaccine.
According to the Division, if a COVID-19 vaccination relates to an employee’s job, and it causes the employee to miss one or more days of work, you should file a First Report of Injury with DWC. Submitting a First Report of Injury to DWC does not mean that a COVID-19 vaccine reaction is work-related or that the insurance carrier is liable for payment. The Division does not clarify what it means when it states that a vaccination must “relate to an employee’s job” for purposes of this reporting. We advise employers to report vaccine injuries, as well as other injuries, when an employee reports any adverse reaction that the employee claims may be work related.
The Division also notes that the IAIABC and the Workers’ Compensation Insurance Organizations (WCIO) have developed new coding guidance for reporting an adverse reaction to a COVID-19 vaccine.
DWC states that carriers should report COVID-19 vaccine reaction claims using the new “nature of injury” code 38 – Adverse Reaction to a Vaccination or Inoculation combined with the “cause of injury” code 83 – Pandemic. Insurance carriers should also clearly indicate whether the claim involves a COVID-19 vaccine reaction in the incident description field by using language such as “COVID-19 vaccine reaction.” The Division specifically states that carriers should not report vaccine reaction claims using “nature of injury” code 83 – COVID-19.
Upcoming COVID-19 Data Call Submission Deadlines
Submissions for the fifth round of data will be due July 30, 2021.
| The Division has directed all selected insurance carriers and insurance carrier groups to provide summary data using the COVID-19 data call reporting forms and instructions. Each selected insurance carrier or group is required to provide one data submission per insurance carrier or group. | Deadline For Submission to DWC |
| COVID-19 exposures and injuries reported to the insurance carrier from December 1, 2019, through June 30, 2021, and payments made on those injuries as of June 30, 2021. | July 30, 2021 |
Insurance carriers and groups must submit the requested data to DWC through the insurance carrier Austin representative’s Secure File Transfer Protocol box no later than 5 p.m., Central time on the date the call is due. If FO&L serves as your Austin Representative, please coordinate your planned data submission with our office through Heather Terrones at hta@fol.com.
Data call submissions are cumulative. They should include all COVID-19 exposures and injuries reported and payments made on these injuries from December 1, 2019, through each applicable date.
Only selected insurance carriers/groups are required to comply with the data call. Selected insurance carriers must provide summary data using the COVID-19 data call reporting forms and instructions. Each selected insurance carrier or group is required to provide one data submission per insurance carrier or group. However, all insurance carriers should maintain injury level data for the injuries reported in this data call and may be asked to submit that data to DWC in the future.
If you have any questions regarding this data call, please contact Steve Tipton, Bobby Stokes or James Sheffield.



