Highlights from the September 2023 Insurance Carrier Quarterly Meeting
On 09/20/2023, DWC held its Carrier Quarterly Meeting.
Nikki Karr, Director of DWC Enforcement, provided a Compliance and Investigations Update. She began by noting that a Deputy Commissioner over DWC Enforcement has not yet been appointed.
In 2023 to date, DWC has received a total of 1332 complaints, broken down as follows:
-
-
- 17 attendance
- 453 communications (failure to timely respond to claimant, failure to contact DWC, failure to contact employer)
- 375 indemnity benefit delivery
- 317 medical benefit delivery
- 103 other
- 67 quality of care.
-
She noted that 67% of these were external referrals, and 43% were internal referrals, and that medical bill issues take up about 25% of DWC’s time. Of those that have been closed to date, 599 were confirmed, 279 received a DWC education letter, and 618 not confirmed.
Insurance carriers were the respondent in the vast majority of complaints received.
Ms. Karr also provided an update on compliance audits. There were 24 total audits initiated in connection with payment of death benefits and lifetime income benefits. She noted the biggest issue with these was the lack of a DWC-3 or an inaccurate DWC-3, leading to inaccurate benefits being paid.
There were 22 total audits initiated for issues surrounding the initial payment of TIBS, and 19 initiated in connection with medical bill processing.
In 2023 to date, the DWC Fraud Unit has received a total of 900 fraud referrals. Of those, 43 cases were opened, 46 were closed, and 2 were referred for prosecution. Of those 2, both individuals were convicted – one was a claimant, and one was an attorney.
With regard to enforcement case status, Ms. Karr reported that 687 cases have been closed, and 268 cases remain pending. 546 cases were closed for carriers, 107 for health care providers, and 34 for “other” (claimants, attorneys, etc.) Of those, 432 were closed by DWC order, 234 were closed with a DWC warning letter, and 21 proceeded to SOAH.
Of those still pending, there are 195 involving Carriers, 39 involving health care providers, and 39 for others.
Ms. Karr discussed Vertafore’s new Sircon payment system, under which approved administrative penalties imposed by DWC and audit billing invoices may now be paid. She requested that Carriers not pay before receiving the final order and invoice from DWC. An account can be created at http://www.sircon.com/products/company/signup/, and questions can be answered by contacting Sircon Customer Services at 877-876-4430.
Finally, she concluded by discussing “Violations to Watch”, and referring specifically to the failure to timely comply with a CCH Decision and Order. Pursuant to Texas Labor Code §410.169 and 28 TAC §142.16, a party is required to comply with a CCH D&O within 20 days of the order becoming final. However, if the CCH D&O involves benefits, a party must comply no later than the fifth day after filing a written request to appeal.
Mary Landrum, the Deputy Commissioner for Health and Safety, provided a very brief health and safety update. She noted health care provider PBO assessment has begun, and that the Office of the Medical Advisor is working with the Medical Quality Review Panel (MQRP) on that.
Santiago Calderon, Director of Designated Doctor Operations, provided a DD Program update. He noted the updated DD rule changes effective April 2023 for DD testing requirements, licensure and renewal, and that effective 6/5/23 the new DWC-32 and 68 went into effect.
Regarding the changes to the DD testing, licensure and renewal requirements, Mr. Calderon indicated there has been an immediate impact. DWC received 55 new DD applications between January and the end of April 2023; DWC has received 117 new DD applications since April 30, 2023; and there are currently 274 doctors on the DD list (78 of whom are MDs and DOs).
They are currently working on the Chapters 133-134 rule changes for billing and reimbursement. Their goal is to have a formal proposal to be published for comment in the coming weeks, and to adopt rule changes by the end of 2023 with an effective date toward the end of the 1st quarter of 2024.
Greg Arendt, the Director of Medical Fee Dispute Resolution, provide an MFDR Update. He discussed disputes generally between 2021-2023, broken down by dispute type:
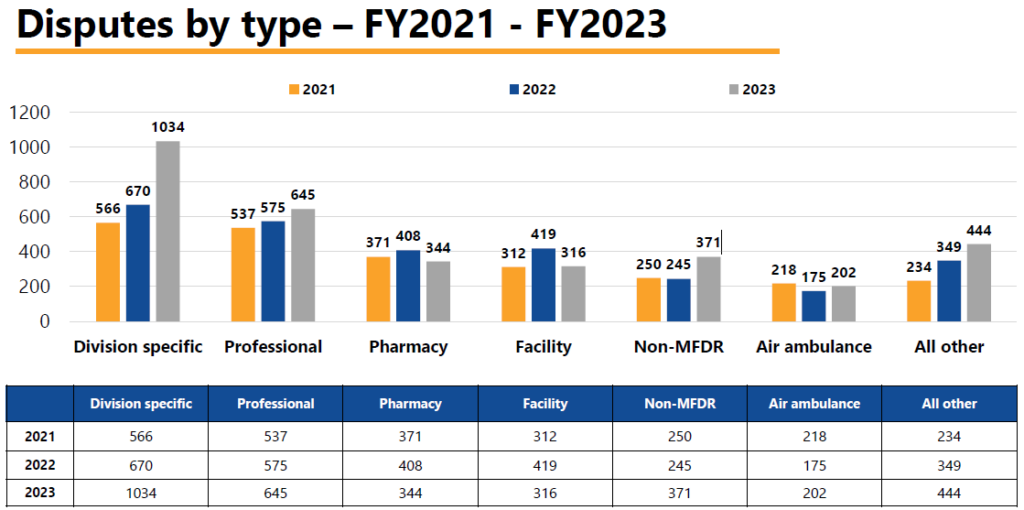
Mr. Arendt then covered various Carrier response issues:
-
-
- 14% of disputes did not receive a carrier response in FY2023.
- Some responses do not meet the requirements of TAC §133.307(d)(2).
- Responses received after 14 days may not be considered in the final dispute decision.
- Responses that include prospective payment for disputed services may be supplemented with proof of payment.
-
Kate Sidora, Director of External and Media Relations provided a legislative update, specifically regarding DWC’s implementation of various bills passed and signed into law in 2023.
The DWC-42 form (Claim for Workers’ Compensation Death Benefits) is being updated, pursuant to HB 2314, which allows for death benefit filing to both carriers and DWC. Information about the proposal should be available in the September 29th Texas Register. She noted the changes are effective for death benefit claims made on or after June 10, 2023.
Regarding HB 2468, the lifetime income benefits (LIBS) bill that changed the traumatic brain injury standard, expanded 3rd degree burns, and implemented changes affecting certain first responders, she said DWC is looking at potential new or updated forms, upcoming rule proposals and adoption. The LIBS topic page and the First Responder FAQ page on the DWC website have both been updated.
Finally, she noted the expiration of the COVID-19 claims presumption, and the recently adopted teledentistry and MQRP rules.
Kara Mace, General Counsel, provided a very brief Legal Services update. She noted various updated to the rules webpage on the DWC website, expanding and making more accessible things such as English and Spanish summaries, comment periods for rules, public hearing information, proposal and adoption orders, and links to the Texas Register.
Kimberly Donovan, Deputy Commissioner of Operations and External Relations, then gave her Research and Evaluation Group (REG) Update.
She provided the following details from their 2023 Return to Work Report:
-
-
- 92% of employees were back at work within 1 year of their injury
- 69% of employees who are back at work within 6 months stay at work
- It takes 2 years for employees who RTW within 6 months to get back to their preinjury wage
- It takes 43 days on average for employees to return to work.
-
REG has upcoming reports pending in the following areas:
-
-
- Pharmacy cost and utilization
- Medical cost and utilization
- Access to care.
-
More information is available at https://www.tdi.texas.gov//wc/reg/index.html.
Martha Luevano, Director for Enterprise Automation Services (EAS), provided an EDI Update.
Regarding Claims EDI R3.1 Implementation:
-
-
- Texas Claim EDI 3.1.4 was implemented on Wednesday, July 26, 2023.
- Claim EDI staff are monitoring PLN 1, PLN 11, and PLN 14 for required EDI reports.
- File a Claim EDI change report to update injured employees IDs, address, phone, and date of injury (do not email DWC.)
- Scorecards and other Claim EDI reports are delayed (will be posted and provided to the registered EDI compliance when complete.)
-
Regarding billing for cost associated with Claim EDI 3.1, she noted:
-
-
- Data collection agent (DCA) may recover start-up costs and ongoing costs.
- Carriers must provide billing contacts to the DCA.
- Governmental entities are excluded.
-
And, with regard to ongoing billing issues:
-
-
- Verisk will soon bill for the remaining half of the one-time costs plus the cost to process the first year of Texas Claim EDI 3.1.4 transactions.
- Memos detailing costs and how invoices are calculated: https://txdwcedi.info/news
- Billing FAQ: https://txdwcedi.info/faq
-
Jeff Nelson, Commissioner of Workers’ Compensation, provided closing remarks. On the topic of designated doctors, he noted DWC lost about 250 DDs between 2018-2022, mainly over complaints about testing and fees. He believes DWC is already seeing improvement – from 239 DDs in January to 274 today.
Finally, Comm. Nelson announced that DWC is going to take a look over the next year at moving from AMA Guides 4th edition to the AMA Guides 6th edition.
Please contact Paul Stone with the firm with any follow up questions regarding September’s Carrier Quarterly DWC meeting: pbs@fol.com.



