CoVID-19 and Telemedicine Highlight Quarterly Carrier Meeting
Senior regulators from the Division of Workers’ Compensation described their initial impressions from the recent CoVID-19 Data Call, their enforcement priorities for the rest of the year and upcoming rulemaking plans during the Carrier Quarterly Stakeholders Meeting that was conducted remotely on August 26, 2020.
Telemedicine Extension
Earlier this month, the Division announced that it would be extending 28 Texas Administrative Code Section 167.1 (Rule 167.1), relating to telemedicine and telehealth. On April 13, 2020, DWC adopted this rule on an emergency basis, and it expires August 10, 2020.
This emergency rule builds on the existing telemedicine and telehealth rules by creating an exception to current CMS distant site practitioner requirements. This rule allows health care providers licensed to perform physical medicine and rehabilitation services, including physical therapists, occupational therapists, and speech pathologists to bill and be reimbursed for services currently allowed under CMS telemedicine and telehealth billing codes.
Many health care providers have made full use of the rule, as demonstrated by Division statistics. Matt Zurek, Deputy Commissioner Health and Safety, noted 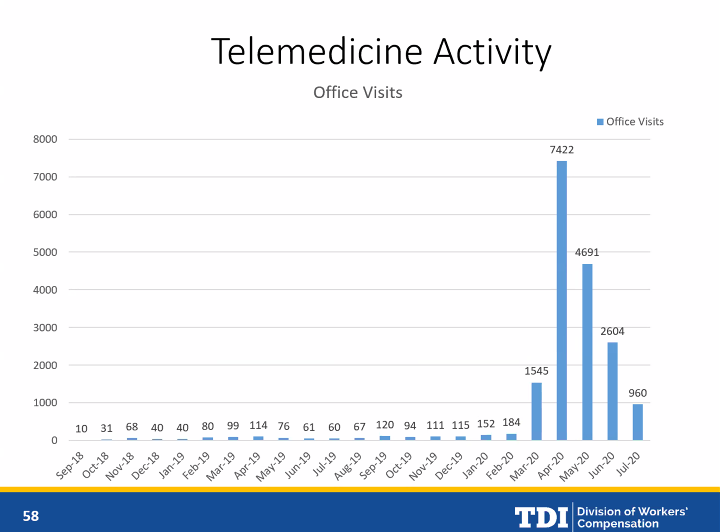 that telemedicine office visits spiked to 7422 in April 2020, shortly after the pandemic hit. There had been barely 1000 such appointments during the whole of 2019.
that telemedicine office visits spiked to 7422 in April 2020, shortly after the pandemic hit. There had been barely 1000 such appointments during the whole of 2019.
Health care providers must bill for telemedicine or telehealth services using the same billing, coding, reporting, and documentation requirements used for in-person services and include a place of service code “02 – telehealth” on the bill. Services will be reimbursed at DWC’s fee schedule rate or network contracted rate, whether provided in person or through telemedicine or telehealth. An originating site facility fee is not eligible for reimbursement.
Under the authority of Government Code Section 2001.034(c), Rule 167.1will be effective through October 8, 2020. Commissioner Brown stated that the agency was reviewing whether to engage in rulemaking to permanently implement the telemedicine changes. She said that no decision had been made in that regard, though.
The telemedicine rule extension notice was published in the August 21, 2020, issue of the Texas Register and is available at www.sos.state.tx.us/texreg/index.shtml.
CoVID-19 Data Call
The agency is pleased with the responsiveness of Carriers who were required to respond to the CoVID-19 Data Call, according to Amy Lee, Special Advisor to the Commissioner and, Director of the Research and Evaluation Group. The first data call deadline was August 17, 2020, and Division staff is reviewing data submissions.
 Ms. Lee said that some carriers are being asked to clarify the data submitted. For example, the Division is attempting to reconcile the number of CoVID-19 claims reported in the data call with the data the Division sees separately in its EDI feed.
Ms. Lee said that some carriers are being asked to clarify the data submitted. For example, the Division is attempting to reconcile the number of CoVID-19 claims reported in the data call with the data the Division sees separately in its EDI feed.
DWC has discovered that some carriers are reporting fewer COVID-19 claims in its EDI data than they are reporting in the data call. This may be because carriers were slow to implement the use of the “nature of injury” code 83 when requested to do so by the Division last spring.
There have been some errors in data submission in this first data call. “Carriers should read the directions” to the data call, said Ms. Lee. “They explain a lot.” Ms. Lee said that there will be at least two more CoVID-19 data calls: October 31, 2020 and January 31, 2021. She does not know whether the Division will add additional data calls to the mix at a later date.
EDI Automation and Transition to Release 3.1
Martha Luevano, Director EDI Automation Services, reminded stakeholders of the necessity of denials including both a paper PLN 1 and an EDI 04. She also emphasized the need to file a medical EDI-03 within five days; if there has been a change in the identity of the carrier’s compliance coordinator or its contact information.
 Ms. Luevano explained that self-reports of EDI violations should no longer be reported to Compliance & Investigations. The self-reports for EDI violations should be sent to edisupport@tdi.texas.gov. Such self-reports should include the description of the issue/violation, the date it was discovered, the number of EDI records affected, the corrective action the carrier is taking and the date the carrier corrects or is scheduled to correct the errors. EDI support staff will respond.
Ms. Luevano explained that self-reports of EDI violations should no longer be reported to Compliance & Investigations. The self-reports for EDI violations should be sent to edisupport@tdi.texas.gov. Such self-reports should include the description of the issue/violation, the date it was discovered, the number of EDI records affected, the corrective action the carrier is taking and the date the carrier corrects or is scheduled to correct the errors. EDI support staff will respond.
Joe McEllrath, Deputy Commissioner for Business Process, told stakeholders to expect an informal rule proposal later this year to change from IAIABC release 1.0 to release 3.1. The Division will be seeking applicants to serve as the agency’s data collection agent for insurance carrier claim data collection in the Release 3.1 format.
Enforcement and Rulemaking
During 2020, there have been 1,053 violation referrals, according to Debra Knight, Deputy Commissioner of Compliance and Investigations. Approximately 50 percent of those referrals concern the failure to timely deliver indemnity or medical benefits.
Ms. Knight said that, while the number of violation referrals are down, the percentage of violations as determined by DWC is increasing. The average monthly payment/processing of (1) medical bill processing of the initial medical bills is around 98 percent compliant, (2) medical bill processing of requests for reconsideration is between 90 and 95 percent, and (3) the initial payment of TIBs is between 80 and 85 %.
Jeb Bodt, a staff attorney explained that the Division still needs to amend a number of rules to make them consistent with 2019 legislative changes. These include (1) rules required by HB 387 which allowed advanced practice RNs to sign DWC 73 work status reports, (2) HB 2503 which expanded eligibility of spouses who may receive death benefits for life, regardless of remarriage to spouses of peace officers and intrastate fire mutual aid system team members or regional incident management team members, (3) SB 1742 which requires the use of same or similar specialty reviewers for UR and IRO reviews, and (4) HB 1665 which eliminated the requirement for hiring contractors to file the DWC 84 with the Division.