Texas WC Commissioner and Staff Address COVID-19 Questions
Texas Commissioner of Workers’ Compensation, Cassie Brown, hosted a Carrier Quarterly Meeting online on May 13, 2020. Among many subjects, the Commissioner and her senior regulatory staff discussed:
-
-
- Ongoing business processes for DD and RME examinations;
- The planned COVID-19 data call;
- Use of telemedicine operations during the pandemic;
- Performance based oversight for 2020;
- Health and safety annual reporting requirements; and
- EDI reporting related to COVID-19 claims.
-
Commissioner Brown opened the meeting by generally describing the agency’s expectations for restarting DD and RME options. In a March 25, 2020 Bulletin, the Division has suspended processes for requesting DD and RME exams until further notice. Commissioner Brown said that such exams will remain suspended canceled until she announces otherwise. She believes that DWC will give the parties sufficient time to pursue the exams once the ban has been lifted. DWC is continuing to collect the DWC 32s and DWC 22s. Her point appeared to be that if the carrier has already filed the document, there is no need to file a second one. However, that fails to account for the 30 day and 10 requirements for a post DD RMEs. Thus, for those requests, we recommend that you refile the DWC-22 after the Division begins approving such examinations again.
generally describing the agency’s expectations for restarting DD and RME options. In a March 25, 2020 Bulletin, the Division has suspended processes for requesting DD and RME exams until further notice. Commissioner Brown said that such exams will remain suspended canceled until she announces otherwise. She believes that DWC will give the parties sufficient time to pursue the exams once the ban has been lifted. DWC is continuing to collect the DWC 32s and DWC 22s. Her point appeared to be that if the carrier has already filed the document, there is no need to file a second one. However, that fails to account for the 30 day and 10 requirements for a post DD RMEs. Thus, for those requests, we recommend that you refile the DWC-22 after the Division begins approving such examinations again.
Commissioner Brown stated that claimants with “special circumstances” may be eligible to obtain a DD examination during the hiatus, but did not elaborate on how those requests would be evaluated. Any such requests will be dealt with on a case-by-case basis.
In response to a question posed by an attendee, Commissioner Brown told participants that nothing has changed regarding performance based oversight for the present time. The Commissioner intends to review the data before making a decision whether to cancel, postpone or reschedule the PBO process. Specifically, Commissioner Brown stated that she wanted to see the data from April to June 2020 before making a decision.
The Commissioner also told attendees to watch for a Bulletin issued around May 14, 2020 that may address changes in preauthorization extensions. The Department of Insurance issued such a bulletin this week was for health insurers. Commissioner Brown expects a WC-specific bulletin will be coming out soon, together with an FAQ.
Joe McElrath, Deputy Commissioner Business Processes, reminded stakeholders that the suspension/cancellation of Division-ordered exams does not apply to exams by treating doctors doing MMI/IR evaluations or to doctors doing MMI/IR evaluations on behalf of the treating doctor.
Mr. McElrath stated that all DD training and certification has been suspended as of April 27, 2020. Some doctors are eligible for interim recertification to perform these exams. Those interim recertification will expire on December 31, 2020. In addition, designated doctor training will be offered virtually beginning September 1, 2020.
Amy Lee, Special Advisor to the Commissioner and Director of the Research and Evaluation Group, noted that the Division has proposed a draft data call on COVID-19 matters. The Research and Evaluation Group will administer the data call. Data results will be published in the Division’s biennial report, December 2020.
The data sought is summary-level information, not claim specific data. The details of the data call have not been finalized, but we anticipate that the Division will seek COVID-19 data at least three separate times this year. These data submissions are designed to reveal how carriers are handling COVID-19 claims. DWC will focus on the following:
-
-
- The number of claimants with COVID-19 reported;
- The number of claimants with confirmed COVID-19 from a positive test or diagnosis;
- The total dollars paid in medical benefits on COVID-19 claims;
- The total dollars paid in income benefits on COVID-19 claims;
- The total dollars paid in death benefits on COVID-19 claims; and
- The total dollars paid in burial benefits on COVID-19 claims.
-
Ms. Lee acknowledged that the data call is expected to present unique issues because of the way government entities collect and report salary continuation for their injured workers.
Ms. Lee emphasized the Division’s belief that the legislature will be very interested in the number of denied claims involving COVID-19. Entities who investigate and evaluate the compensability of COVID-19 claims are well advised to be able to distinguish claims involving reported exposure only (exposure-only claims) from claims involving an actual diagnosis of the disease. If exposure-only claims are denied, this may have the effect of inflating an entity’s overall denial rate.
Martha Luevano, the newly appointed Director EDI Automation Services reminded carriers of their responsibilities to report COVID-19 claims using new diagnosis code 83. This will assist in the identification and review of pandemic claims.
Ms. Luevano stated that while there was “no legal requirement to report exposure claims without a diagnosis,” the Division is encouraging employers to make these reports. She stated that the agency’s COVID-19 resource page should have a new FAQ on this subject soon.
We recommend that employers consult with their respective carriers before making any decision to report claims that are not legally required to be reported.
In a major announcement involving EDI claims reporting, Ms. Luevano stated that the Division is strongly considering whether DWC should move from IAIABC Release 1 to IAIABC Release 3. The Division plans to issue informal rule proposal this summer to do this. Carriers have been reporting under IAIABC Release 1 since 1995.
Chris D’Amura, Director Workplace Safety, reminded stakeholders that their annual accident prevention reporting requirements have not been suspended. He stated that a late report is better than no report at all and encouraged carriers who have not yet completed that reporting to do so promptly. Mr. D’Amura also mentioned that DWC is handling virtual consultation visits for OSHA Consultation. His workgroup conducted 18 such visits in April 2020.
Debra Knight, Deputy Commissioner for Compliance & Investigations, oversees (1) Audits & Investigations; (2) Fraud; and (3) Enforcement. Ms. Knight stated that DWC has received 687 complaints this year, which is down from prior years. The most common complaints against carriers are as follows : (1) late TIBs and IIBs payments ; (2) late initial payment of TIBs : (3) failure to pay the correct TIBs rate ; (4) failure to investigate a claim ; and (5) failure to timely comply with a CCH decision and order or a medical fee dispute resolution finding and decision.
Deputy Commissioner for Health & Safety Matt Zurek discussed telemedicine issues. He noted that Rule 133.30, which became effective May 8, 2016, creates an exception to Medicare payment policy restrictions for telemedicine for certain services. On April 13, 2020, the Division passed Emergency Rule 167.1 that applies telemedicine to physical medicine and rehabilitation services. The emergency rule will be in effect for 120 days, but it may be extended by another 60 days. T
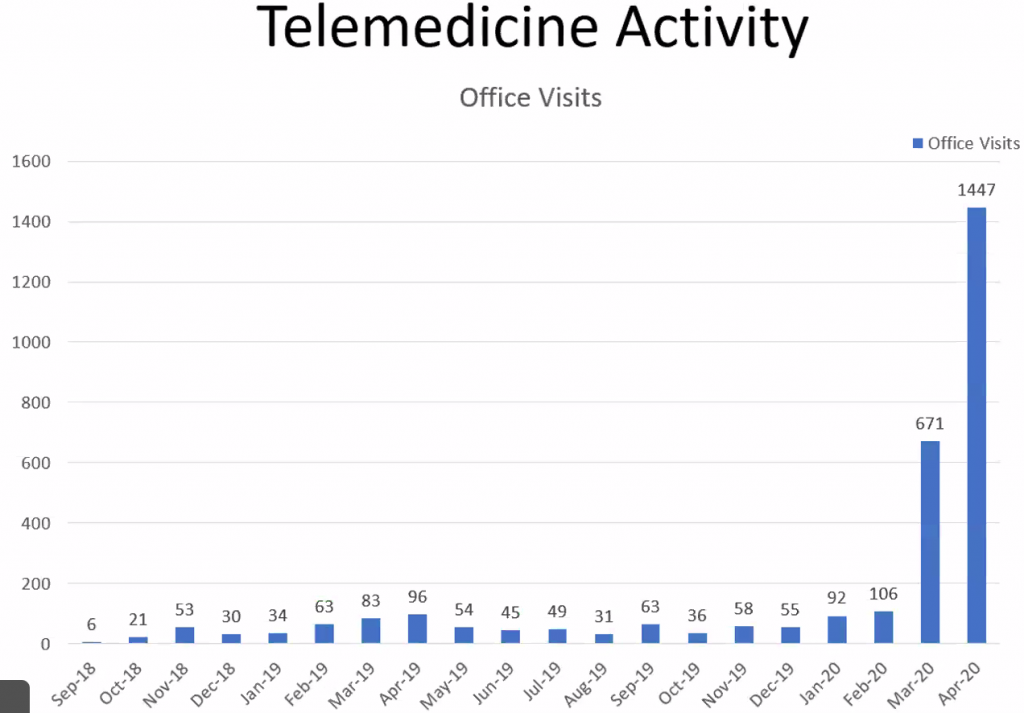 Mr. Zurek stated that the most frequently reported codes involving telemedicine are low back pain, sprains/strains of the low back, lumbar radiculopathy, chronic pain syndrome, shoulder pain and knee pain. In the last two months, there has been a large spike in telemedicine services. Before March 2020, telemedicine bills were hovering below 100 per month. In March, they increased to 786, and to 1,714 in April. About 75 % of the telemedicine services are being provided by MDs and DOs.
Mr. Zurek stated that the most frequently reported codes involving telemedicine are low back pain, sprains/strains of the low back, lumbar radiculopathy, chronic pain syndrome, shoulder pain and knee pain. In the last two months, there has been a large spike in telemedicine services. Before March 2020, telemedicine bills were hovering below 100 per month. In March, they increased to 786, and to 1,714 in April. About 75 % of the telemedicine services are being provided by MDs and DOs.
Greg Arendt, Director Medical Fee Dispute Resolution, reminded stakeholders that if a carrier’s denial of medical benefits during a medical fee dispute is compensability or liability or extent of injury, the carrier must produce a PLN 1 or a PLN 11 to support its EOBs.



