Use of Telemedicine in Texas Comp Spiked During Pandemic
Use of telemedicine increased significantly as the COVID-19 pandemic tightened its grip on Texas workers. But new research indicates utilization of the service is on the decline. Overall, the utilization of telemedicine services was higher during the pandemic than before the pandemic.
In 2017, the Texas Legislature passed a comprehensive bill addressing telemedicine in Texas, specifically removing certain limitations on its use. The Division of Workers’ Compensation’s telemedicine rule, designed to support the legislative change, took effect September 1, 2018. A new research report shows that the use of telemedicine services in the Texas workers’ compensation system remained low until March 2020 when Governor Abbott’s COVID-19 disaster declaration took effect. The services significantly increased after the DWC passed an emergency rule in April 2020. As the effects of the global pandemic has begun to wane, so has use of telemedicine in the workers’ compensation system.
In Evaluation of Telemedicine Services in the Texas Workers’ Compensation System: 2018-2021, researchers from the Texas Department of Insurance Workers’ Compensation Research and Evaluation Group identified six key findings regarding telemedicine:
Percentage of Claims: Less than 1 percent of claims receiving professional medical services received telemedicine pre-pandemic but increased to 7 percent of claims during the pandemic.
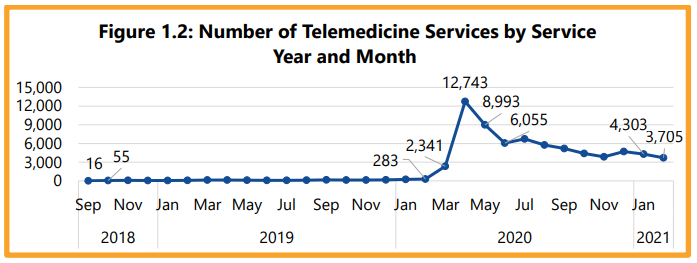
Utilization: Telemedicine utilization was low until March 2020 when the pandemic began. Utilization increased again as DWC’s emergency rule 28 TAC §167.1 took effect in April 2020. This expanded access to telerehabilitation services, but when Texas began reopening, there was a rapid decline in the use of these services.
Demographics: During the pandemic, more men and older injured employees received telemedicine services.
Type of Service: Office visits were the most frequently used telemedicine service before and during the pandemic.
Cost: Total payments for telemedicine services increased during the COVID-19 pandemic. Insurance carriers paid about three-fourths of billed services.
Days from Injury: The average number of days from injury to initial telemedicine service was about six to seven weeks from April to September 2020, but decreased in 2021 to about three weeks.
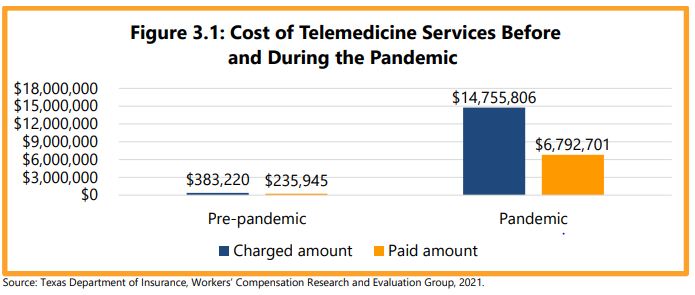
 From September 1, 2018, through July 31, 2021, health care providers billed for 80,613 telemedicine services and 76 percent of these services were paid by insurance carriers. The total amount charged by health care providers for these telemedicine services was $15,139,026. The insurance carriers paid a total of $7,028,646, or 46 percent of the total charged amount. As shown in Figure 3.1, the amount charged and paid for telemedicine services was much higher during the pandemic than before, even though fewer months were covered during the pandemic. The amount charged was $14,755,806 for telemedicine services during the pandemic with 46 percent ($6,792,701) paid by insurance carriers. Before the pandemic, the amount charged was $383,220, but a higher percentage of these charges were paid (62 percent, $235,945).
From September 1, 2018, through July 31, 2021, health care providers billed for 80,613 telemedicine services and 76 percent of these services were paid by insurance carriers. The total amount charged by health care providers for these telemedicine services was $15,139,026. The insurance carriers paid a total of $7,028,646, or 46 percent of the total charged amount. As shown in Figure 3.1, the amount charged and paid for telemedicine services was much higher during the pandemic than before, even though fewer months were covered during the pandemic. The amount charged was $14,755,806 for telemedicine services during the pandemic with 46 percent ($6,792,701) paid by insurance carriers. Before the pandemic, the amount charged was $383,220, but a higher percentage of these charges were paid (62 percent, $235,945).
 Telemedicine – typically defined as a doctor or health care professional using computer or electronic video systems to examine a patient at another location – was historically limited by Medicare based reimbursement restrictions relating to “underserved” areas, which are typically rural regions with insufficient access to health care providers, and must be provided in a doctor’s office, hospital, or certain clinics.
Telemedicine – typically defined as a doctor or health care professional using computer or electronic video systems to examine a patient at another location – was historically limited by Medicare based reimbursement restrictions relating to “underserved” areas, which are typically rural regions with insufficient access to health care providers, and must be provided in a doctor’s office, hospital, or certain clinics.
The DWC rule eliminated the Medicare based reimbursement restrictions that limit the use of telemedicine in workers’ compensation to these underserved areas. That allowed the use of telemedicine everywhere in Texas. The rule also eliminated the Medicare based requirement that the telemedicine service be provided in a doctor’s office, hospital, or certain clinic. Instead, an injured employee could be physically located anywhere at the time they receive telemedicine services.
The Division maintains a telemedicine page on its website. In addition, the Division has published an FAQ page specifically devoted to telemedicine issues and questions. As more providers consider the application of telemedicine in their practices, we are receiving questions regarding what kinds of services may be furnished via telemedicine. Note the following Q&A from the DWC FAQ page:
Q: Can any medical service be delivered via telehealth/telemedicine?
A: No. The Division adopts, by reference, the list of telehealth services published annually by Medicare.
You can find a list of covered telehealth services published by Medicare for CY 2018 and CY 2019 at this link. DWC has adopted Medicare coding, billing and documentation policies by reference. Medicare policies that conflict with the Division’s adopted rules do not apply.
This new research report presents baseline information about the utilization and cost of telemedicine services in the Texas workers’ compensation system before and during the COVID-19 pandemic. The REG states it is important to monitor the utilization and cost of these services as the pandemic continues, and whether these services are being done in medically underserved geographic areas in the state. The use of telemedicine by network vs. nonnetwork claims is also an area for future research since networks are in a better position to promote the use of telemedicine services with contracted health care providers and enrolled injured employees.